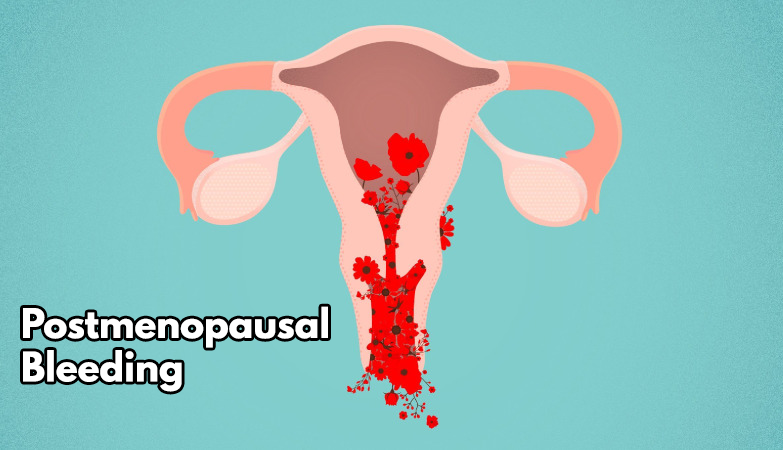
Introduction to Postmenopausal Bleeding
Ever heard of the phrase, “Expect the unexpected?” Well, that’s kind of how our bodies work, especially when it comes to women’s health. As we journey through the roller coaster of life, there are things we think we understand, only for our bodies to throw a curveball.
“OR”
Postmenopausal bleeding is bleeding that occurs after menopause. Menopause is a stage in a woman’s life (around age 51) when reproductive hormones drop and her monthly menstrual periods stop. Vaginal bleeding that occurs more than a year after a woman’s last period isn’t normal. The bleeding can be light (spotting) or heavy.
Postmenopausal bleeding is usually due to benign (noncancerous) gynecological conditions such as endometrial polyps. But for about 10% of women, bleeding after menopause is a sign of uterine cancer (endometrial cancer). Uterine cancer is the most common type of reproductive cancer (more common than ovarian or cervical cancers.) Talk to your healthcare provider if you experience any bleeding after menopause.
What is Menopause?
Menopause marks a significant milestone in a woman’s life. It’s when her menstrual cycle permanently comes to a halt, typically around the age of 50. But did you know that it’s not just about saying goodbye to monthly periods?
What to Expect After Menopause?
Post menopause, while periods cease, there are still changes and symptoms that can occur, such as hot flashes and mood swings. But what if you suddenly experience bleeding again? It’s a little like seeing rain in a desert, right?
Postmenopausal Bleeding
Definition and Basics
Postmenopausal bleeding refers to bleeding from the reproductive system after a woman has been menopause-free for over a year. Think of it like getting a call from a number you’ve long deleted!
Causes of Postmenopausal Bleeding
Why does this happen? It’s like planting seeds in a barren land and expecting a tree, isn’t it?
Common Causes
- Vaginal atrophy
- Endometrial atrophy
- Polyps
Less Common Causes
- Endometrial cancer
- Infections
Importance of Early Detection
Catching it early is like realizing your sink is leaking before your entire kitchen is flooded. It can save you a lot of trouble and lead to a more effective solution.
Diagnosing Postmenopausal Bleeding
Physical Examination
Your doctor is your detective here, searching for clues to get to the root of the mystery.
Ultrasound and Endometrial Biopsy
An ultrasound is like taking a sneak peek, while an endometrial biopsy is akin to diving deep underwater for treasures.
Hysteroscopy Procedure
Imagine a small camera navigating a maze; that’s hysteroscopy for you!
Treatment and Management
There’s always light at the end of the tunnel, and solutions are at hand.
Hormonal Treatment
Balancing hormones is akin to finding equilibrium on a seesaw.
Surgical Options
Sometimes, a more direct approach, like removing a stumbling block from your path, is necessary.
Lifestyle Changes and Recommendations
You’re the captain of your ship. Simple tweaks to your lifestyle can change the course of your journey.
Conclusion
Our bodies are filled with surprises, and postmenopausal bleeding is one such unexpected visitor. Awareness, timely detection, and appropriate treatment are keys to navigating this phase smoothly. Remember, every cloud has a silver lining, and this too shall pass.
Frequently Asked Questions
- Is postmenopausal bleeding always a sign of cancer?
No, while it can be a sign, many benign conditions can also cause bleeding.
- How is postmenopausal bleeding diagnosed? A combination of physical examination, ultrasound, biopsy, and sometimes hysteroscopy.
- Can lifestyle changes reduce the risk of postmenopausal bleeding?
Yes, a balanced diet, regular check-ups, and managing stress can help.
- Are there any non-surgical treatments for postmenopausal bleeding?
Yes, hormonal treatments are often the first line of defense.
- Should I consult a doctor even if the bleeding is minimal?
Absolutely. It’s always better to be safe than sorry.